Airway Obstruction in Infants and Children
Upper airway obstruction in children is dangerous and may progress
rapidly. It is essential to make a firm diagnosis and take the appropriate
action without delay.
139
SIGNS OF AIRWAY OBSTRUCTION
1 Stertor is the noise produced by obstruction in the throat, i.e. above the
larynx, and is usually a low-pitched choking type of noise.
2 Stridor is a high-pitched sound produced by narrowing within the more
rigid confines of the larynx or trachea. In laryngeal obstruction the stridor
is inspiratory; in tracheal lesions it is usually both inspiratory and
expiratory.
3 Use of accessory muscles of respiration.
4 Pallor, sweating and restlessness.
5 Tachycardia.
6 Cyanosis. It is important to examine the child in adequate lighting,
preferably daylight.The lips particularly will show the dusky coloration,
which may be very subtle.
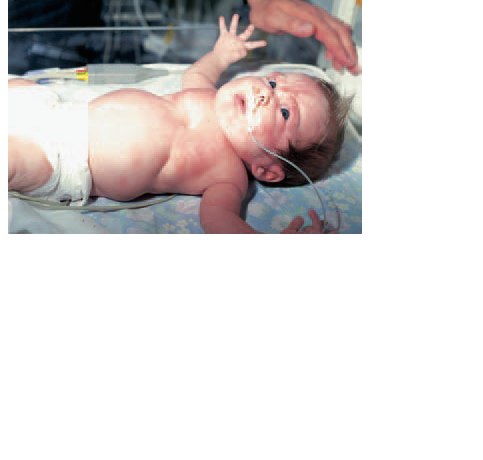
7 Intercostal and sternal recession (Fig. 37.1).The sternum may be sucked
in almost to the vertebrae in the child’s attempts to breathe.
8 Exhaustion—a late stage in asphyxia,which should be avoided.The
child makes less effort to breathe, stridor and insuction become less
pronounced and apnoea is not far off.
Box 37.1 Signs of airway obstruction.
Management of airway obstruction
The management of airway insufficiency always depends on the severity of
the obstruction, and severe obstruction necessitates immediate airway
support by oxygen, endotracheal intubation or even tracheostomy.
If time and the child’s condition allow, every child with stridor should
have a PA chest X-ray and a lateral soft-tissue film of the neck, which will
show the larynx and upper trachea clearly. If a vascular ring or tracheooesophageal
fistula is suspected, a barium swallow is a necessary investigation
Neonates may be intubated without the need for general anaesthesia
but great care must be taken not to damage the larynx and cause further obstruction
from haematoma or oedema. Older children, unless so anoxic as
to be unconscious, will require general anaesthesia for intubation, and at
the same time the larynx, trachea and bronchi should be inspected. The
diagnosis is then usually apparent and further management can be directed
appropriately.
LARYNGOSCOPY AND BRONCHOSCOPY
Inspection of the airways in cases of respiratory obstruction calls for the
highest degree of cooperation between surgeon and anaesthetist.
The larynx is inspected under deep anaesthesia using a rigid paediatric
laryngoscope and Hopkins rod telescope (Fig. 37.2). An anaesthetic type
laryngoscope usually gives an inadequate view owing to its poorer lighting.
Bronchoscopy in babies and children has been facilitated greatly by the
introduction of ventilating bronchoscopes, which allow coupling to a Tpiece
anaesthetic circuit and at the same time provide superb vision
through a rod-lens telescope system (Fig. 37.3). A side channel allows for instrumentation
and suction. Using this type of bronchoscope, the airways of
even small premature babies may be examined with a much greater degree
of precision and safety than is possible with the older type open bronchoscope
tube.
Causes of upper airway obstruction in infancy
SUPRA LARYNGEAL CAUSES
Choanal atresia
Failure of posterior canalization of the nasal airways results in severe neonatal
airway obstruction, which is relieved by crying. Surgical correction will
be required.
Micrognathia
Underdevelopment of the mandible as in Pierre Robin syndrome or
Treacher–Collins syndrome results in posterior displacement of the
tongue and oropharyngeal obstruction.The neonate may asphyxiate unless
corrective measures are taken.
Adeno-tonsillar hypertrophy
Large tonsils and adenoids may occlude the naso-oro-pharyngeal airway
to a serious degree, especially during sleep. This may result in obstructive
apnoea during sleep, with loud snoring punctuated by periods of silence
followed by a large gasp. If not recognized and treated, right heart failure may ensue.
LARYNGEAL CAUSES
Congenital
Laryngomalacia (Fig. 37.4)
The stridor starts at or shortly after birth and is due to inward collapse of
the soft laryngeal tissues on inspiration. It usually resolves by the age of 2 or
3 years, but meanwhile the baby may have real respiratory difficulties. Diagnosis
is confirmed by laryngoscopy without intubation when the supraglottic
collapse is seen on inspiration. It can be relieved by division or excision of
the aryepiglottic folds.
Congenital subglottic stenosis
This occurs at the level of the cricoid cartilage.There will be stridor from
birth and the stenosis may be visible on a lateral X-ray of the neck. Diagnosis
is confirmed by laryngoscopy.
Laryngeal webs
Laryngeal webs are anteriorly situated (Fig. 37.5) and if large can cause severe stridor and obstruction.The most extreme degree of webbing, atresia,
is fatal unless immediate tracheostomy is performed.
Laryngeal cysts
Laryngeal cysts may be congenital or may be the result of endotracheal
intubation. They may cause variable airway obstruction, often dependent
on position.
Vascular ring
A vascular ring developmental anomaly of the aorta—surrounds the oesophagus
and trachea, causing constriction. Diagnosis is made by barium
swallow and angiography, and the treatment is by surgery to divide the vascular ring.
Acquired
Foreign body (Figs 37.6 and 37.7)
The sudden onset of stridor in a formerly normal child must always be regarded
as being due to a foreign body until proved otherwise. A history of
choking and coughing, especially if while eating, should alert the attending
doctor to the likelihood of aspiration; peanuts are particularly dangerous in
this respect and should never be given to youngsters. Examination and chest
X-rays may be entirely normal and the only way to exclude a foreign body in
the bronchus is by bronchoscopy.
A larger foreign body may lodge in the larynx and cause severe respiratory
distress. It may be possible to remove it by the Heimlich manoeuvre
(compression of the upper abdomen to raise intrathoracic pressure) but if
this fails, endoscopy or tracheostomy will be necessary.
Acute laryngitis,acute epiglottitis and laryngotracheobronchitis
Described in Chapter 33.
Subglottic stenosis (Fig. 37.8)
Subglottic stenosis is now seen most commonly in low-birth-weight babies
who have required prolonged ventilation by endotracheal tube, but may
occur at any age from intubation or trauma.Treatment is highly specialized
and entails some form of laryngotracheoplasty. Subglottic stenosis cannot
always be avoided.
Multiple laryngeal papillomata (Fig. 37.9)
Multiple laryngeal papillomata should be suspected in a child with progressive
hoarseness or aphonia and airway obstruction. There may be little stridor since the mass of papillomata is too soft to vibrate the air column.
Diagnosis is by direct laryngoscopy, and removal of the papillomata is best
accomplished using the carbon dioxide laser, which is very accurate and, if
used carefully, causes least damage.The papillomata are of viral origin (HPV
6 or 11) and have a strong tendency to recur.
NB. Any child with stridor is potentially at risk of dying from
asphyxia and every case should be investigated to determine the
cause. It is dangerous to believe that all children ‘grow out’ of a tendency to stridor.


